Conditions Treated
Venous reflux (also called chronic venous insufficiency) occurs when one way valves in the leg veins weaken and fail to function properly, causing blood to flow backward and pool in the lower limbs. This increased venous pressure can lead to leg heaviness, swelling, cramps, and varicose veins.
Over time, untreated venous reflux may result in skin discolouration or even venous ulcers. Early diagnosis with duplex ultrasound and minimally invasive treatments such as endovenous radiofrequency ablation can restore healthy circulation and prevent long-term complications.
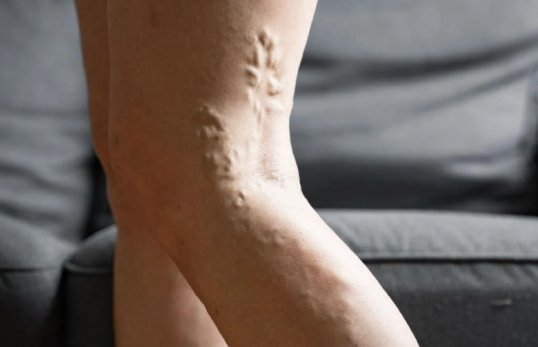
Varicose veins are enlarged, bulging leg veins caused by weakened vein valves and chronic venous insufficiency. Symptoms can include leg heaviness, cramping, swelling, and visible ropey, bluish veins. Although often considered cosmetic, varicose veins are very much a medical condition because they can signal underlying venous reflux.
If left untreated, they may progress to skin changes or venous ulcers. Diagnosis is usually with duplex ultrasound. Modern minimally invasive treatment often combines modalities (e.g. radiofrequency ablation, sclerotherapy, and mini phlebectomies) to improve symptoms and appearance.
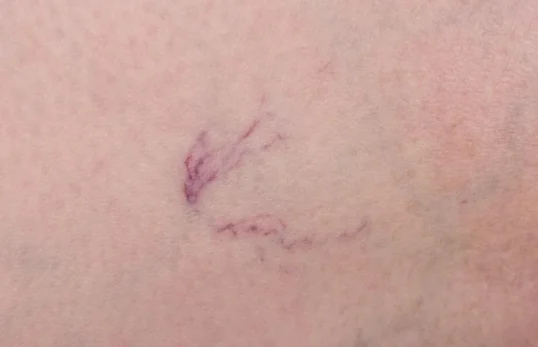
Spider veins (also called telangiectasia) are tiny red, blue, or purple thread-like veins close to the skin surface. They most often appear on the calves, ankles, or face. They are usually painless, but some people notice mild itching or a burning sensation.
Although often cosmetic, spider veins can sometimes suggest underlying venous reflux, especially if you also have leg heaviness, swelling, or night cramps. Seek assessment if they spread quickly, cause persistent symptoms, or if there are skin changes around the ankle. Diagnosis is by clinical review and, when needed, duplex ultrasound. Treatment may include sclerotherapy, VeinGogh ohmic thermolysis, or laser.
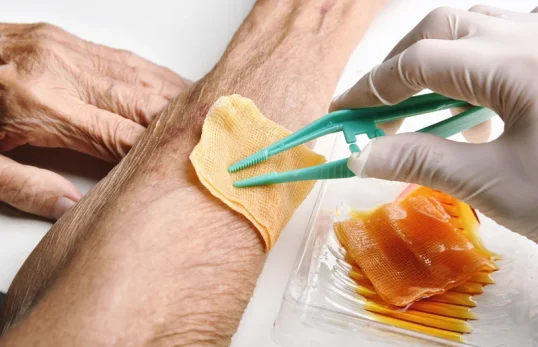
Poorly healing wounds are chronic ulcers or sores (often on the foot or leg) that fail to improve within the expected timeframe. Common causes include poor blood circulation (peripheral arterial disease), diabetes, infection, and chronic venous insufficiency. Reduced blood flow prevents oxygen and nutrients from reaching the tissue and supporting normal repair.
Seek assessment early if you have redness, pus-like drainage, swelling around the wound, or persistent pain. Early vascular assessment (e.g. duplex ultrasound) is important to identify underlying causes. Treatment focuses on addressing the cause, infection control, debridement, advanced wound dressings (e.g. negative-pressure therapy), and improving blood flow when required.
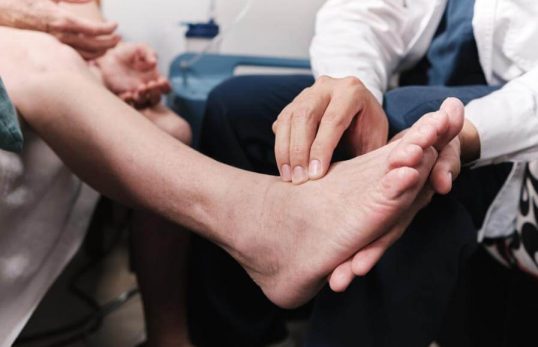
Peripheral vascular disease (PVD) is reduced blood flow to the legs due to narrowing or blockage of the leg arteries. It is often caused by atherosclerosis and increases overall cardiovascular risk. Patients may experience calf cramps when walking that ease with rest (claudication), numbness, cold feet, poorly healing foot wounds, or even gangrene.
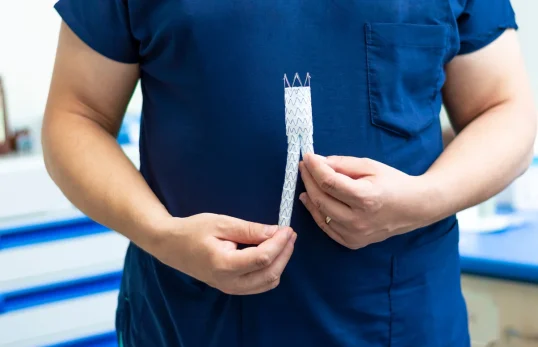
Diagnosis is usually with duplex ultrasound (and sometimes CT angiography). Treatment depends on symptoms and severity, ranging from risk-factor optimisation and lifestyle changes to minimally invasive angioplasty and stenting to restore blood flow.
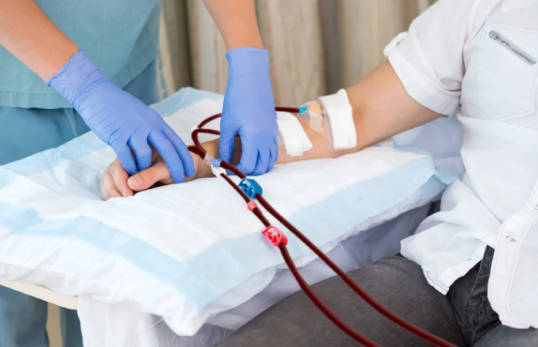
Dialysis access is the specialised blood-vessel connection used for haemodialysis, usually an arteriovenous fistula (AVF) or arteriovenous graft (AVG). A well-functioning access is essential for effective dialysis and long-term treatment. Potential problems include poor maturation, low flow, blockage, infection, bleeding, aneurysm/pseudoaneurysm, and hand pain or coldness (steal syndrome).
Seek early assessment if the thrill feels weaker, the arm becomes swollen, bleeding lasts longer after dialysis, or cannulation becomes difficult. Assessment is with clinical review and ultrasound. Treatment is often minimally invasive (angioplasty/stenting), though open surgery may sometimes be needed.
Aortic aneurysm is a widening (ballooning) of the aorta, the body’s main artery. It may occur in the abdomen (AAA) or chest (TAA). Many aneurysms cause no symptoms and are found on health screening or unrelated scans, but the key risk is enlargement and rupture.
Seek urgent attention for sudden severe chest, back, or abdominal pain, especially if you have a known aneurysm. Diagnosis is usually with ultrasound or CT angiography. Management depends on symptoms, size, and growth rate. Treatment ranges from surveillance and risk-factor control to endovascular stent grafting (EVAR/TEVAR) or open surgery when indicated.
Pelvic congestion syndrome (PCS), also called pelvic venous insufficiency, occurs when pelvic veins (often the ovarian veins) become dilated and reflux, causing blood to pool and pressure to build up around the uterus and ovaries. It commonly causes a persistent dull lower abdominal or pelvic ache (often lasting >6 months), usually worse after prolonged standing and sometimes during or after intercourse, and it may radiate to the lower back or thighs.
Seek assessment if pelvic pain is unexplained or if you notice vulval or upper-thigh varicose veins. Diagnosis is with duplex ultrasound and, when needed, venography. Treatment strategies may include minimally invasive embolisation of the refluxing pelvic veins.
Deep venous thrombosis (DVT) is a blood clot in a deep vein, usually in the leg, which can block blood flow and cause swelling and pain. Typical symptoms include one-sided leg swelling, calf tenderness, warmth, and redness or skin discolouration. DVT matters because part of the clot can travel to the lungs and cause a life-threatening pulmonary embolism.
Seek urgent care if leg symptoms occur with sudden breathlessness, chest pain, or coughing up blood. DVT is usually diagnosed with duplex ultrasound. Treatment is typically anticoagulation, with selected cases needing minimally invasive clot-removal procedures such as thrombectomy or thrombolysis.