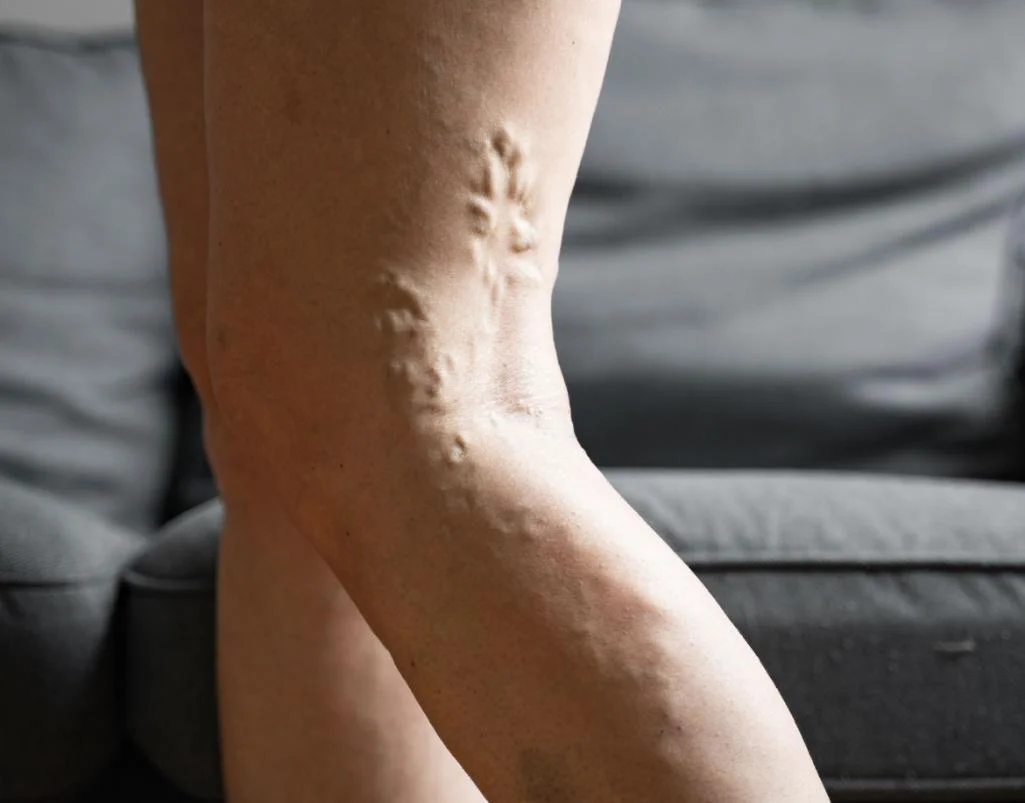
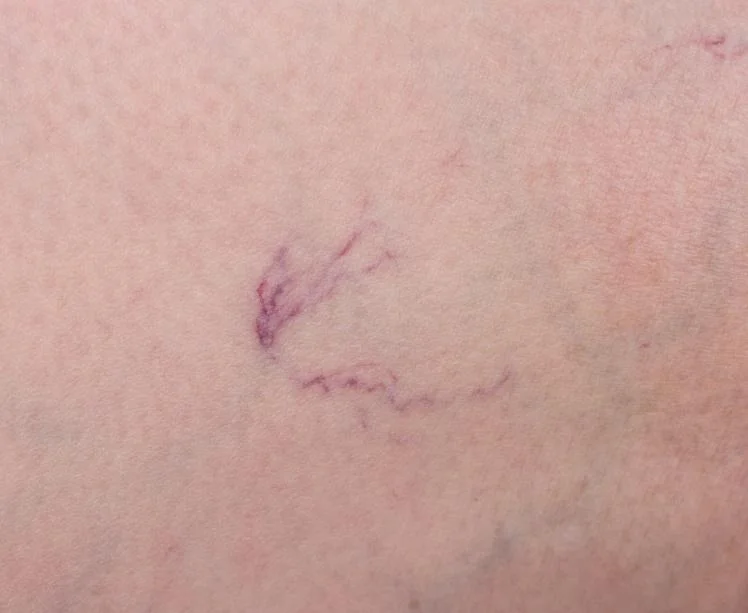
Radiofrequency ablation (RFA) and VenaSeal are two of the most popular minimally invasive vein surgery options for treating varicose veins. They both work by closing off faulty veins to redirect blood flow to healthier ones, but they do so in different ways. Choosing between the two often comes down to your anatomy, lifestyle, and medical considerations.
Let’s break down the differences to help you decide which might be the best vein treatment for you.
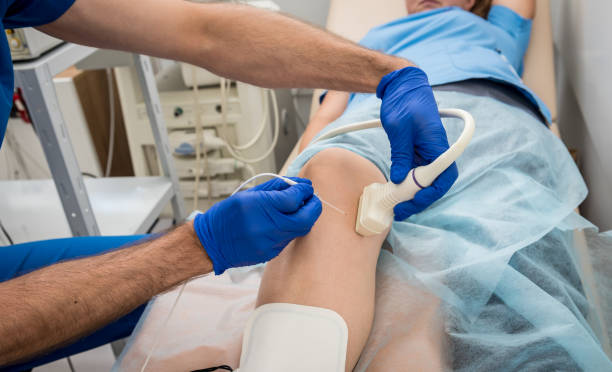
How Do These Treatments Work?
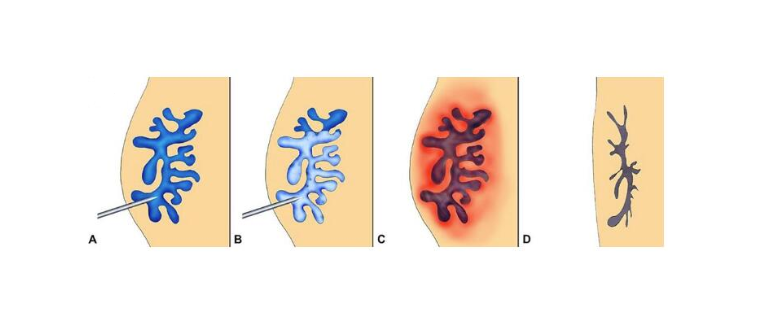
Radiofrequency Ablation (RFA) uses heat energy to close off the problem vein. A thin catheter is inserted into the vein, and radiofrequency energy is applied to seal it shut. It’s a tried-and-tested method with excellent long-term results.
VenaSeal is a newer technique that uses a medical adhesive (a type of bio-glue) to seal the vein shut. Instead of heat, it relies on a safe, cyanoacrylate-based glue to close the vein from the inside, with no need for thermal energy.
Key Differences Between RFA and VenaSeal
| Feature | Radiofrequency Ablation (RFA) | VenaSeal |
| Technique | Thermal (heat-based) | Medical adhesive (glue) |
| Anaesthesia | Local anaesthesia or light general anaesthesia | Usually requires only local anaesthesia |
| Compression Stockings | Worn for 1–2 weeks after the procedure | Often not required |
| Pain/Discomfort | Mild discomfort or bruising common | Mild discomfort; no heat application |
| Recovery Time | Back to normal in 24–48 hours | Back to normal in 24–48 hours |
| Post-Procedure Care | Some aftercare needed (stockings, activity restrictions) | Minimal post-procedure care |
| Suitability | Excellent for most patients | Not ideal for very superficial veins or those prone to adhesive reactions |
| Risks | Bruising, tenderness, nerve injury, skin irritation | Hypersensitivity, allergic reaction, nerve injury, local skin changes |
| Long-Term Data | Over 20 years of clinical use with robust long-term outcomes | Newer, with growing but limited long-term data (under 10 years) |
| Success Rate | 90–98% at 5 years | Approximately 94–95% at 5 years |
| Cost | Typically more cost-effective | Generally more expensive due to adhesive material |
Effectiveness and Long-Term Results
When comparing radiofrequency ablation vs VenaSeal, both offer strong long-term closure rates and symptom relief.
- RFA has been in use for over two decades and boasts success rates of around 90–98% in five years. It’s considered the gold standard for thermal vein treatments.
- VenaSeal is newer but shows similarly high success rates — approximately 94–95% — in clinical trials and real-world use.
Both are considered safe, effective options for minimally invasive vein surgery, and recurrence rates are low when performed by experienced hands.
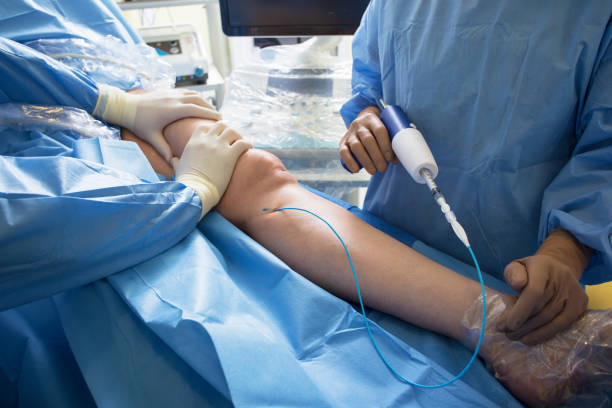
Pros and Cons at a Glance
| Radiofrequency Ablation (RFA) | VenaSeal | |
| Pros | – Proven long-term outcomes – Widely available – Cost-effective – Suitable for most vein types | – No compression stockings needed (in most cases) – Minimal downtime – Very little post-op discomfort – No thermal injury risk |
| Cons | – Requires compression stockings – May cause bruising or tenderness – Not ideal for very small or tortuous veins – Minor risk of nerve injury | – Higher cost – Not suitable for very superficial or tortuous veins – Risk of hypersensitivity or allergic reaction – Limited long-term data (under 10 years) – Possible local irritation in superficial veins |
So, Which One Is Better?
There’s no single “best vein treatment” — it really depends on your individual case. If you’re looking for a proven, cost-effective option with strong long-term data, radiofrequency ablation is an excellent choice. If you’re after a more comfortable recovery and want to avoid compression stockings, VenaSeal may be the better fit.
Some patients may even benefit from a combination of treatments, depending on how many veins are affected and their specific anatomy.
Final Thoughts
Both RFA and VenaSeal offer safe, effective, and minimally invasive solutions for treating varicose veins. The key is choosing the treatment that best fits your vein condition, lifestyle, and personal preferences.
Dr Darryl Lim is a vascular surgeon in Singapore with experience in both RFA and VenaSeal procedures. If you’re considering treatment for varicose veins, he can help guide you through your options and tailor a plan that’s right for you.
FAQ
Is VenaSeal better than radiofrequency ablation?
Both are highly effective. VenaSeal offers a faster recovery, but RFA has a longer track record. The best choice depends on your veins and your goals.
Which vein treatment is less painful?
VenaSeal is generally associated with less post-procedure discomfort, as it doesn’t use heat.
Do I have to wear compression stockings after treatment?
After RFA, yes — usually for 1 to 2 weeks. With VenaSeal, compression stockings are often not required.