Diabetes is a growing concern worldwide, and Singapore is no exception. With diabetic foot complications being among the most serious and disabling, proper management is crucial. If not handled correctly, these complications can lead to severe outcomes such as ulcers, infections, and even amputations. This guide will help you understand the causes, management, and prevention of diabetic foot complications, providing valuable insights for those at risk.
Diabetic Statistics in Singapore
Diabetes is a significant health issue in Singapore. Approximately 14.9% of the adult population, or about 711,800 people, are living with diabetes. The prevalence of diabetes is expected to rise, with projections indicating an additional 200,000 cases by 2030, bringing the total number to around 600,000 residents aged 40 and above. In response to this growing epidemic, the Singapore government launched the “War on Diabetes” campaign in 2016, spearheaded by then-Prime Minister Lee Hsien Loong.
Causes of Diabetic Foot Complications
Diabetic foot complications primarily arise from diabetic neuropathy, peripheral vascular disease (PVD), and a weakened immune system.
Diabetic Neuropathy
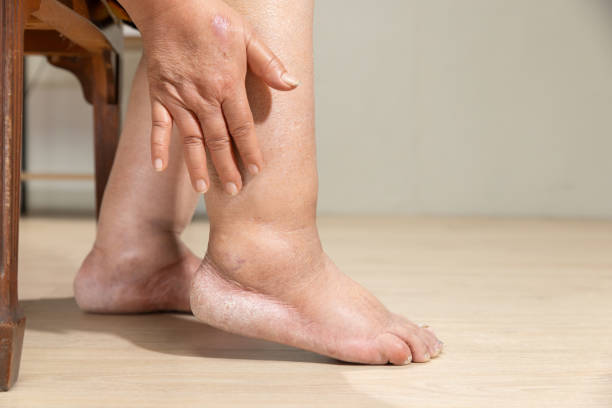
Diabetic neuropathy is a major contributor to foot complications. When diabetes damages the nerves, it leads to reduced sensation in the feet. This means injuries can go unnoticed and untreated, leading to serious issues. Neuropathy can also cause foot deformities, like hammertoe and Charcot’s foot, which increase pressure points and result in skin breakdown and ulcers. Additionally, decreased nerve function affects sweat glands, causing dry, cracked skin that’s more prone to infections.
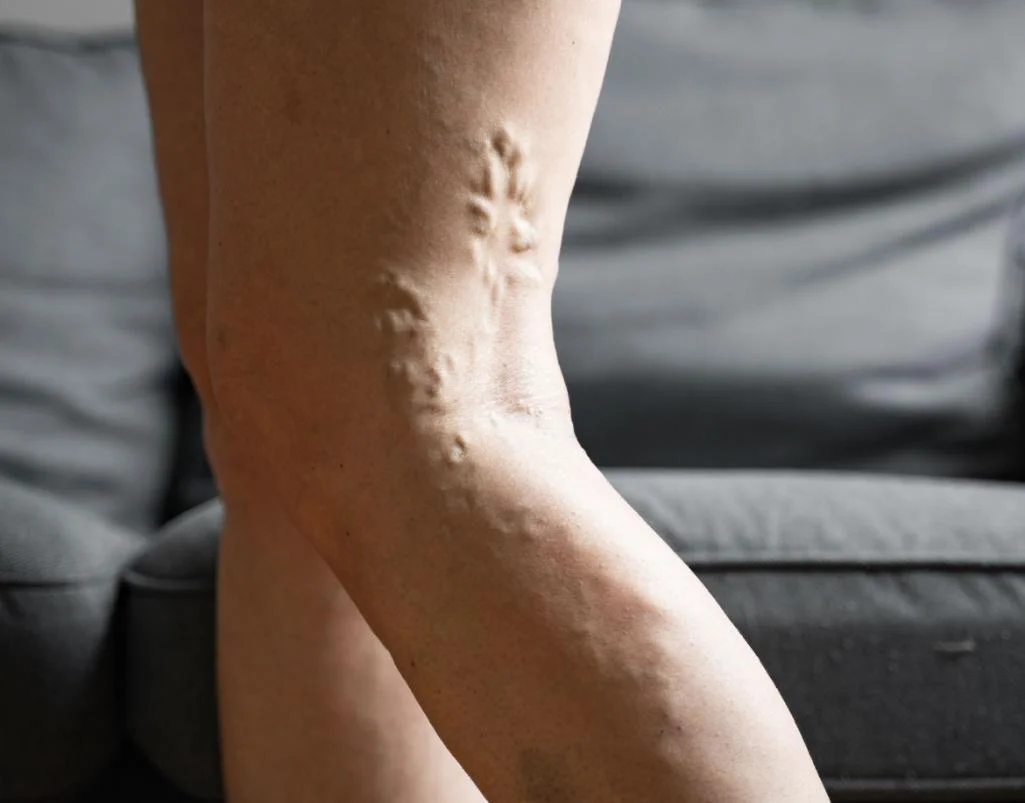
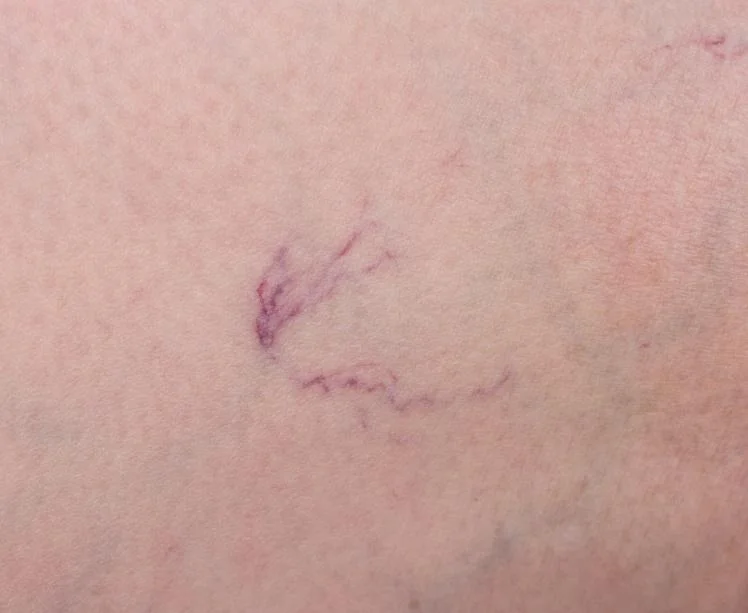
Peripheral Vascular Disease (PVD)
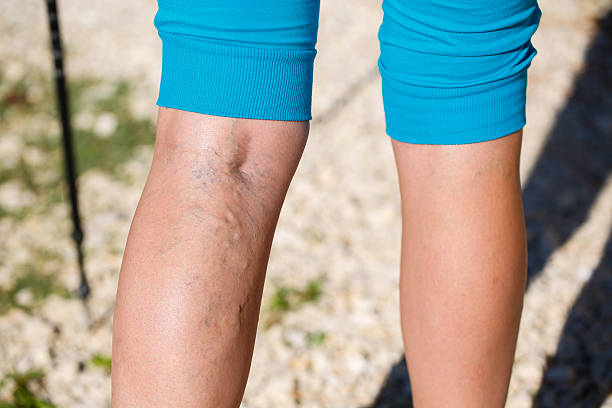
PVD involves the narrowing and hardening of the arteries in the legs, a condition known as atherosclerosis. This reduces blood flow, hindering wound healing and significantly increasing the risk of infection. Approximately 70% of diabetic wounds are associated with PVD, and nearly 85% of diabetes-related amputations are preceded by an ulcer. Early detection and intervention are crucial to preserving the function of your lower limbs.
Weakened Immune System
Diabetes impairs the immune system, making it harder for the body to fight infections. Small foot injuries can quickly become serious if left untreated due to this reduced immunity.
Managing Diabetic Foot Complications
Effective management of diabetic foot complications involves several key strategies.
Ensuring Adequate Blood Supply
Adequate blood supply is essential for healing and preventing severe complications. Diagnostic tools such as ultrasounds or CT angiograms are used to assess blood flow. Treatment options include surgical bypass or endovascular techniques like balloon angioplasty to improve circulation.
Infection Control
Recognizing and addressing infections promptly is vital. Signs of infection include redness, swelling, foul odor, pus, and pain. Systemic signs can include fever and fatigue. Treatment typically involves antibiotics based on culture and sensitivity testing. More serious cases might require surgical intervention, such as wound debridement, to remove infected tissue.
Wound Care
Proper wound care is crucial for healing. This often involves debridement, the surgical removal of non-viable or infected tissue, and using appropriate dressings to maintain a moist environment and minimize contamination.
Offloading Pressure
Reducing pressure on ulcers and sores is key to healing. Specialized footwear can help redistribute pressure, and in severe cases, crutches or wheelchairs might be necessary. Our in-house podiatrist can provide full consultations to tailor the best solutions for your needs.
Preventing Diabetic Foot Complications
Preventing complications involves managing risk factors and adopting healthy lifestyle habits.
Risk Factor Management
Maintaining good blood sugar control is paramount, as high levels damage nerves and blood vessels. Managing blood pressure and cholesterol levels also helps reduce the risk of atherosclerosis.
Lifestyle Modifications
Smoking cessation is critical, as smoking exacerbates circulation problems and interferes with the wound healing process.
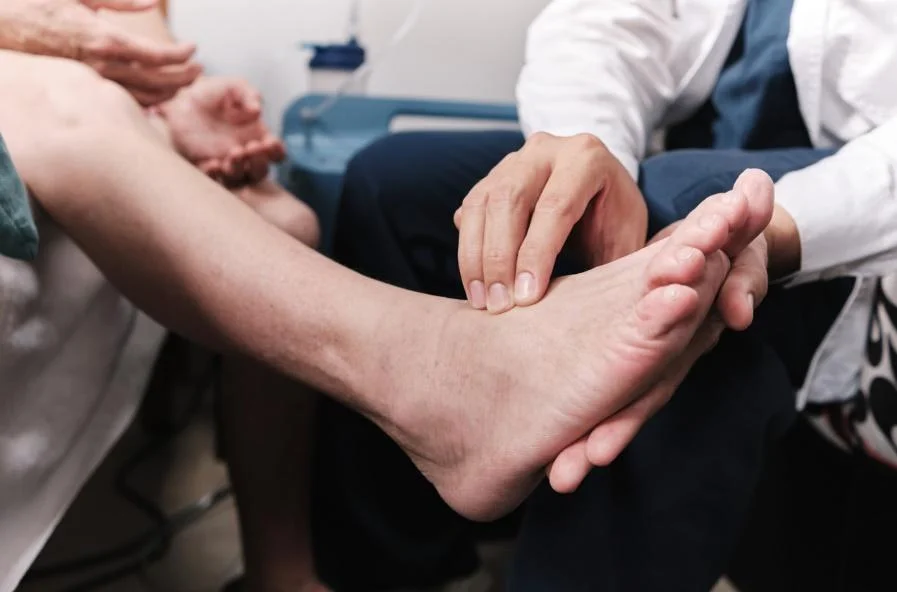
Foot Care
Daily foot inspections are essential. Check for cuts, sores, and blisters regularly, and avoid going barefoot. Choose well-fitting shoes, and our in-house podiatrist can customize appropriate footwear for your condition. Keeping your feet clean and moisturized helps prevent cracks and infections.
Dealing with Diabetic Foot Problems?
Diabetes can lead to serious foot complications if not addressed early. Get expert care to protect your feet and prevent further issues.

Conclusion
Understanding and managing diabetic foot complications are crucial to preventing severe outcomes like amputations. Regular check-ups, proper foot care, and effective diabetes management can significantly reduce the risk. If you experience any unusual symptoms in your feet, consult a healthcare provider promptly.
Dr. Darryl Lim is one of the few doctors in Singapore accredited as a Certified Wound Specialist Physician (CWSP) by the American Board of Wound Management. He is highly experienced in minimally invasive techniques for treating Peripheral Vascular Disease and frequently trains emerging interventionalists in the region. Dr. Lim boasts one of the region’s best limb salvage rates, consistently above 90%, a testament to his skill and dedication in this field. His expertise in wound care, combined with advanced revascularization techniques like angioplasty and stenting, significantly improves the chances of successful wound healing and amputation prevention for patients facing these challenges. For more information and personalized advice, visit Dr. Darryl Lim’s clinic.