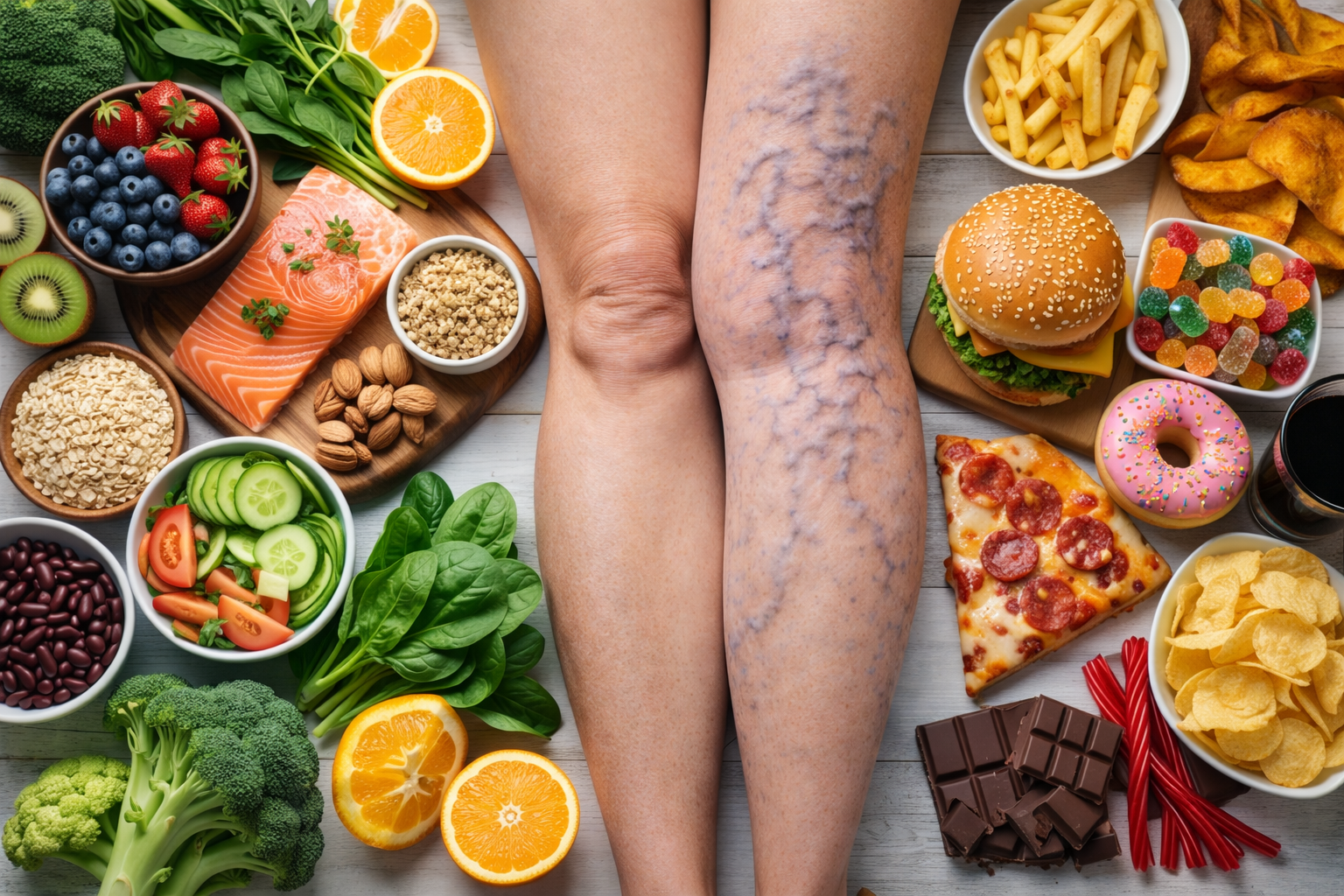
Varicose veins are often dismissed as merely a cosmetic issue, but they can indicate more serious vascular problems. These visible signs of vein malfunction should not be ignored, as they can lead to significant health complications if left untreated. Understanding when to seek medical advice is crucial for effective treatment and prevention of serious outcomes.
Understanding Varicose Veins
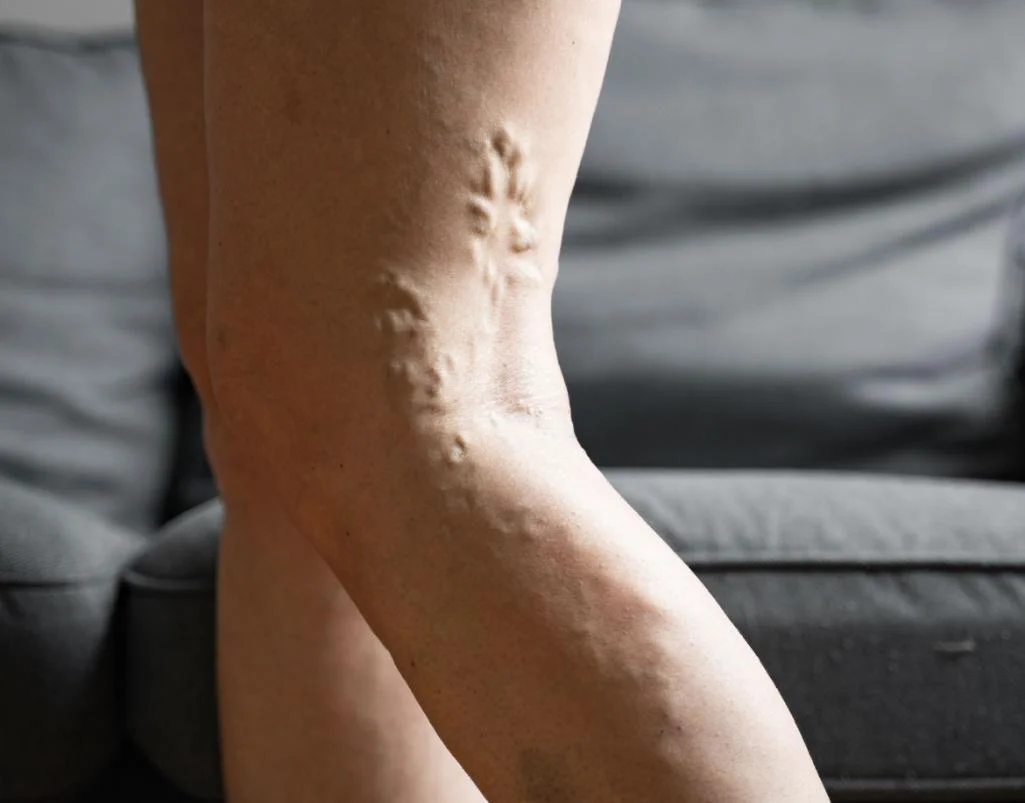
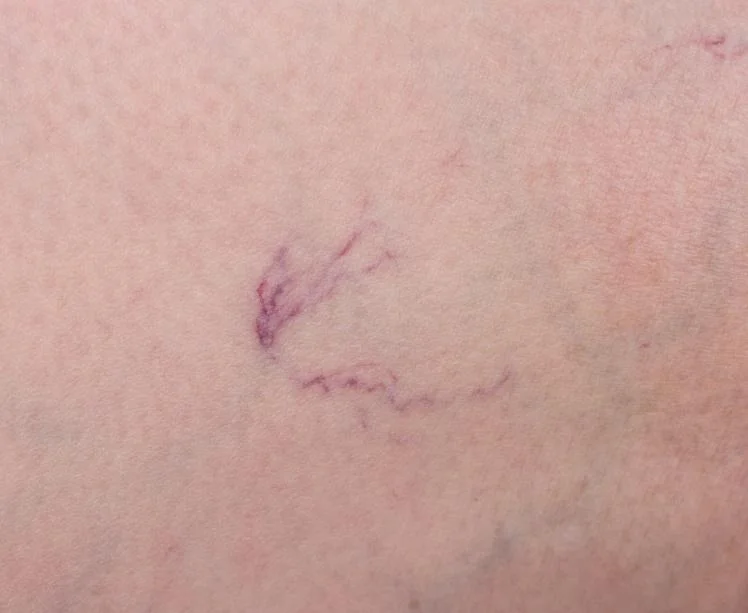
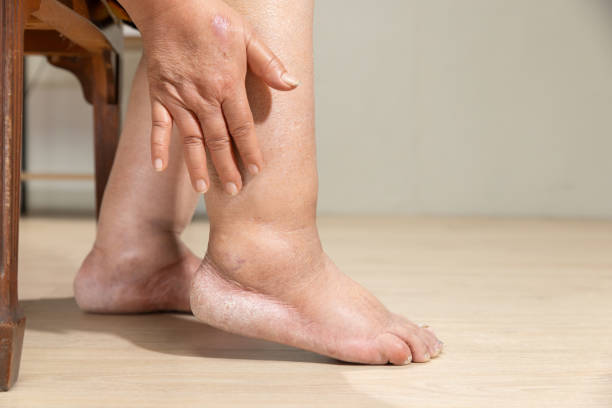
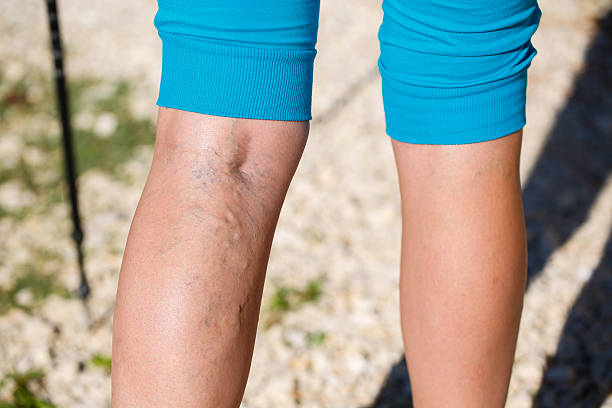
Varicose veins are swollen, twisted veins visible just beneath the surface of the skin, usually appearing in the legs and often blue or purple in color. While they might seem harmless at first glance, varicose veins can cause discomfort and signal underlying vascular issues that require medical attention.
Symptoms that warrant a doctor’s visit
Certain symptoms suggest a need for medical evaluation. If your legs constantly feel painful or heavy, especially after standing for extended periods, this persistent discomfort can interfere with daily activities and reduce your quality of life. Noticeable changes in the color or texture of the skin, such as darkening or the development of skin ulcers near your ankles, can indicate serious vascular problems that should not be ignored. Significant swelling in the legs or ankles could signal vascular complications that need professional attention, often accompanied by a feeling of heaviness or tightness.
Advanced Complications to Watch for
Severe complications from varicose veins are rare but require immediate medical attention. Varicose veins near the surface of the skin can bleed if injured, and even a minor bump or scratch can cause significant bleeding due to the increased pressure in these veins.
Thrombophlebitis, involving a blood clot forming in a vein leading to inflammation and pain, can cause redness, swelling, and tenderness in the affected area, necessitating prompt medical intervention.
A more serious condition, Deep Vein Thrombosis (DVT), involves a blood clot forming in a deeper vein, usually in the legs, and requires urgent treatment to prevent complications like pulmonary embolism, where the clot travels to the lungs.
Preventive Measures and Treatment Options
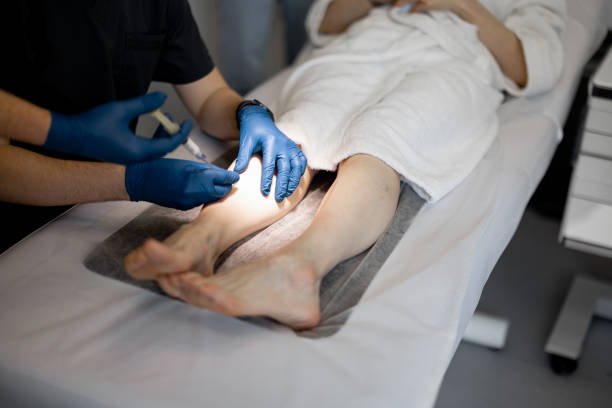
Preventive care and early treatment can significantly improve your quality of life. Regular exercise, maintaining a healthy weight, and avoiding prolonged periods of standing or sitting can help prevent the development of varicose veins. Wearing compression stockings can also alleviate symptoms and improve circulation. For more persistent or severe cases, medical procedures like sclerotherapy, where a solution is injected into the vein to close it, or surgical options such as vein stripping, might be necessary. These treatments are designed to reduce symptoms and prevent complications.
Struggling with Varicose Veins?
Explore safe and effective treatment options with Dr. Darryl Lim.

Conclusion
If you’re experiencing any of the above symptoms or if your varicose veins are causing discomfort, don’t hesitate to seek professional advice. Early intervention is key to managing symptoms effectively and avoiding complications. Living with varicose veins can be painful and may lead to more serious health issues if left untreated. By consulting with a vascular specialist, you can get a personalized treatment plan that addresses your specific needs, preventing the progression of the disease and improving your overall vascular health. Whether you’re experiencing mild discomfort or more severe symptoms, getting expert advice is crucial. Contact Dr Darryl Lim today to schedule an appointment with a vascular specialist and take the first step towards improving your health and well-being.