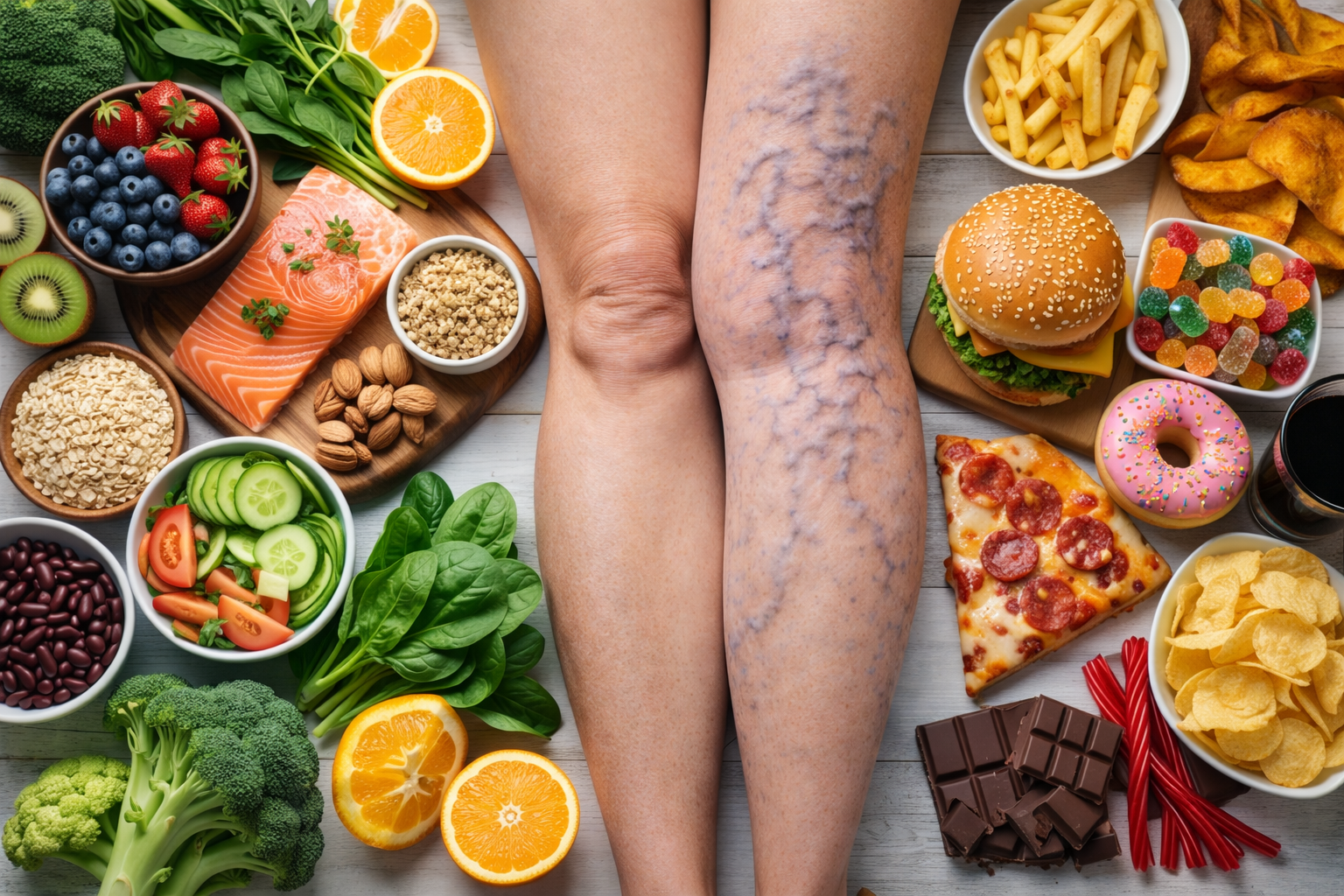
It often starts subtly. You lie down after a long day expecting rest, but instead your legs begin to ache. Sometimes it’s a dull heaviness. Other times it’s that crampy, tight feeling in the calves that makes you shift around in bed, or a sudden spasm that jolts you awake.
Night-time aching or crampy legs are common, but if it’s happening regularly, it’s worth paying attention to the pattern rather than brushing it off.
In this guide, Dr Darryl Lim, a vascular and varicose vein specialist in Singapore, explains 8 common causes of lower leg pain at night, how to tell which ones are more likely, and when it may signal an underlying circulation issue that should be checked.
Why leg symptoms often feel worse at night
During the day, movement helps circulation. Walking activates your calf muscles, which push blood upwards towards the heart.
At night:
- You’re no longer moving, so the calf muscle pump slows
- Any swelling or venous pooling from the day becomes more noticeable
- Muscle tightness and crampy sensations are more likely to surface when you finally rest
- Nerve symptoms and inflammation can feel louder in stillness
Now let’s go through the most common causes.
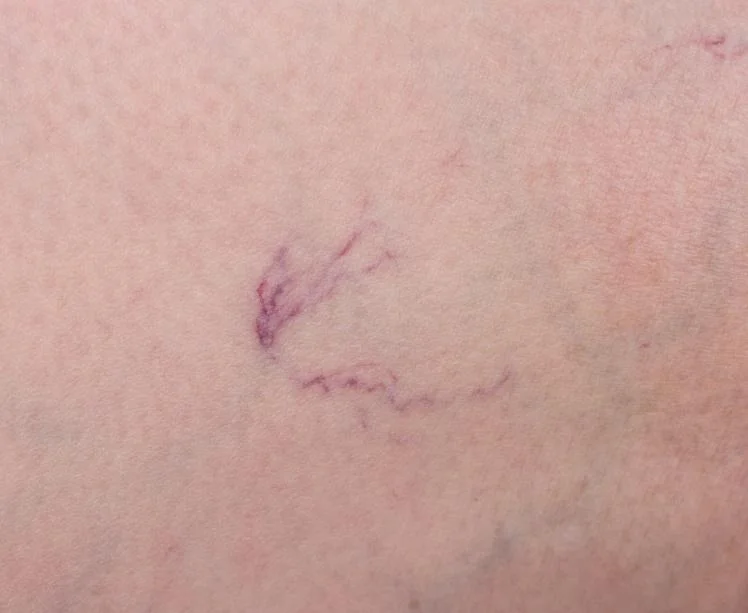
1) Chronic venous insufficiency (Venous Reflux)
One of the most overlooked causes of aching or crampy legs at night is chronic venous insufficiency. This happens when vein valves don’t close properly, allowing blood to fall backwards (venous reflux) and pool in the lower legs.
Symptoms often build up through the day, especially after long periods of standing or sitting, because gravity encourages pooling around the ankles and calves. The ache or crampy tightness then becomes most noticeable at night- not because lying down makes it worse, but because you’re finally still and you’re feeling the day’s accumulated venous pressure. By morning, many people feel better as a night of lying flat takes gravity out of the equation and gives the ankles a chance to decongest.
Typical symptoms include:
- Heavy, aching legs at night (often after a day of standing)
- A dull throbbing sensation in the calves
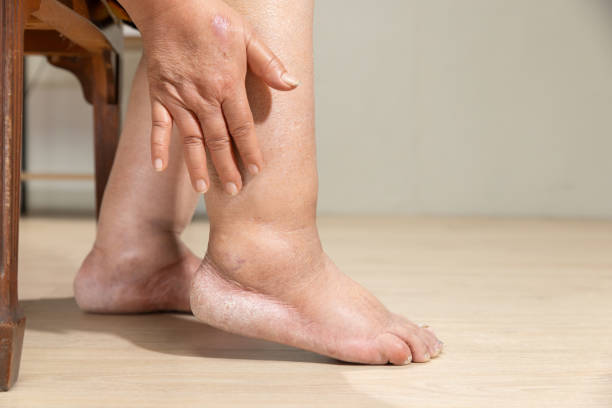
- Ankle swelling
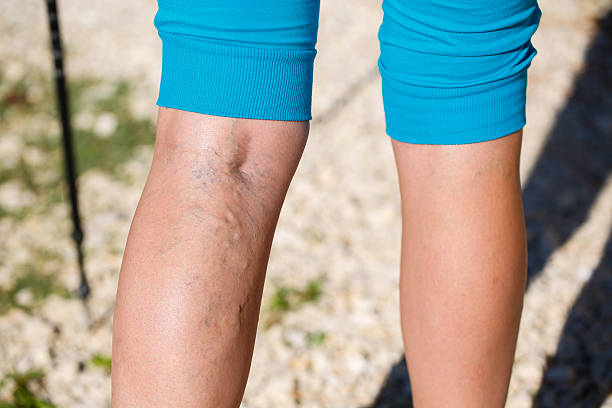
- Visible varicose veins
- Itching or tightness around the lower leg
- Skin changes such as brown ankle discolouration or eczema-like patches
Some people call this “crampy” because the legs feel tight, restless, and uncomfortable (especially at bedtime), after a long day on their feet.
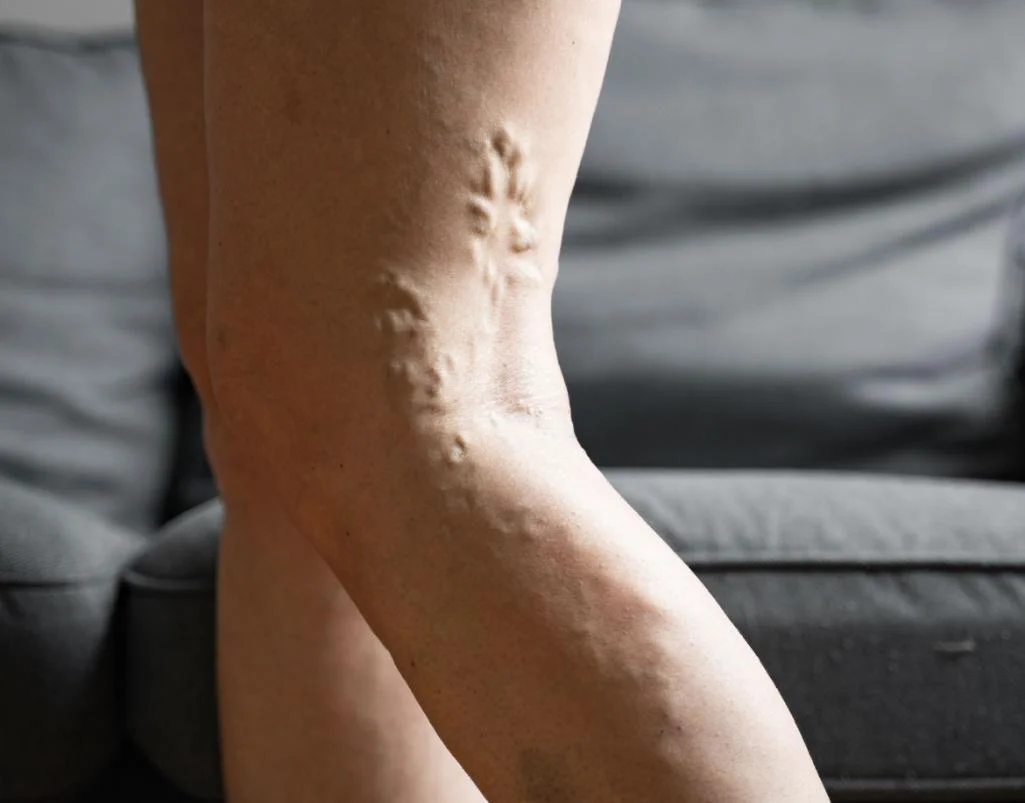
2) Varicose veins
Varicose veins are enlarged, twisted surface veins. In most cases, they are not just a surface problem– they reflect the same underlying issue as chronic venous insufficiency: weak vein valves and venous reflux, which increases pressure in the superficial veins and causes them to dilate over time.
Night symptoms linked to varicose veins can feel like:
- Dull aching
- A pressure sensation
- Pulsing discomfort
- Burning along the vein
- A crampy heaviness after long standing days
Symptoms often worsen after prolonged standing (or long hours sitting) and become more noticeable in bed, because venous pooling and pressure have built up through the day. If you also have ankle swelling, heaviness, or skin changes, it strengthens the likelihood that underlying venous reflux (CVI) is driving the symptoms.
3) Nocturnal leg cramps
This is the classic “crampy legs at night” problem. Nocturnal leg cramps are sudden, intense muscle contractions (often in the calf). They can:
- Wake you from sleep
- Cause sharp, stabbing pain
- Leave lingering soreness the next day
Common triggers include:
- Dehydration
- Excess sweating
- Overexertion
- Pregnancy
- Prolonged standing
- Some medications (for example, diuretics may contribute via electrolyte shifts)
Unlike venous aching, cramps are usually abrupt and intense rather than slow-building heaviness.
4) Peripheral artery disease (PAD)
Peripheral artery disease involves narrowed arteries that reduce blood flow to the legs. Night pain from PAD tends to feel different from vein-related aching.
Typical clues:
- Pain is often in the feet or toes, not just the calf
- It may worsen when legs are elevated
- It may improve when you sit up or let the legs hang down
Venous aching often improves with elevation, while arterial “rest pain” can worsen with elevation.
PAD should be assessed promptly and more urgently if you have diabetes, a smoking history, non-healing wounds, or pain at rest.
5) Restless legs syndrome
Restless legs syndrome causes uncomfortable sensations and an urge to move the legs, and it’s often mistaken for “cramps” at first.
People describe:
- Crawling or “antsy” sensations
- Tingling
- Pulling or electric feelings
Symptoms typically worsen in the evening and at night, and improve temporarily with movement.
RLS is primarily neurological rather than vascular, but chronic venous insufficiency (venous reflux) can sometimes contribute to a similar “restless” or crampy leg feeling, especially after long periods of standing or sitting. Some patients have both conditions- and if you also notice ankle swelling, visible varicose veins, or ankle itching/discolouration, it’s worth considering an assessment for venous reflux as well.
6) Muscle overuse or strain
A long day of walking, standing, or exercise can cause delayed-onset muscle soreness (DOMS), and it can absolutely feel crampy at night when the muscles cool down.
Typical features:
- Generalised tenderness
- Bilateral calf discomfort
- Tight, crampy calves
- Pain with movement or going downstairs
- A clear link to recent activity
This usually improves over a few days with rest, hydration, and gentle stretching.
7) Nerve compression (Sciatica)
Lower back issues can cause nerve pain that radiates into the lower leg.
This may feel like:
- Sharp, shooting pain
- Burning
- Numbness or tingling
- Pain that worsens in certain positions (including lying flat)
Unlike venous symptoms, nerve pain often follows a more predictable path from the back or buttock down the leg.
8) Electrolyte imbalance (and hydration issues)
Low levels of minerals such as magnesium, potassium, or calcium can contribute to cramping and nighttime discomfort in some people.
Common causes include:
- Dehydration
- Excess sweating
- Certain medications
- Poor diet or low intake
If cramps are frequent and persistent, blood tests can help clarify whether there’s an underlying deficiency or medication-related cause.

Quick comparison: Venous vs Arterial vs Nerve pain (a simple self-check)
More likely venous (CVI / varicose veins) if:
- Worse after standing all day
- Heavy, aching, throbbing sensation
- Crampy tightness with swelling or visible veins
- Ankle swelling present
- Visible veins or ankle skin changes
- Often improves with leg elevation and walking
More likely arterial (PAD) if:
- Pain in feet/toes, especially at rest
- Symptoms worsen when legs are elevated
- Improved by hanging legs off the bed
- Cold feet, poor healing wounds, reduced walking distance
More likely nerve-related if:
- Burning/shooting pain, pins-and-needles
- Numbness
- Clear radiation pattern from back/hip down the leg
- Triggered by posture
At the end of the day, the pattern usually gives you a pretty good clue about what’s going on.
When to seek medical evaluation
Consider an evaluation if you experience:
- Persistent nightly aching or crampy legs
- Swelling that doesn’t settle
- Brown ankle discolouration or eczema-like skin changes
- Visible varicose veins with pain
- Symptoms that regularly interfere with sleep
Seek urgent medical assessment if you have:
- Severe leg/foot pain with a cold, pale, or blue foot
- Foot or leg wounds that aren’t healing
- New weakness or numbness in the leg or foot (especially if sudden)
- Sudden, marked one-sided swelling with redness/warmth
- Shortness of breath or chest discomfort
Need an expert vascular opinion for your Varicose Veins?
Book an appointment with Dr. Darryl Lim today and get a personalized treatment plan.
How lower leg pain is properly diagnosed
A proper assessment depends on the likely cause, but may include:
- Clinical examination
- Venous reflux duplex ultrasound (to assess valve function and presence of venous reflux)
- Arterial duplex ultrasound (if arterial disease is suspected)
- Assessment of neurological or musculoskeletal causes where relevant
If leaky veins are suspected as a cause, ultrasound is the key test to confirm reflux and map which veins are involved.
Simple steps that may reduce aching or crampy legs at night
If you’re looking for something practical you can do tonight, start here:
Try elevating your legs for 15–30 minutes before bed, and aim for regular walking during the day- even short walks make a difference. Stay well-hydrated, especially if you sweat a lot, and do a bit of gentle calf stretching in the evening. If you’ve been sitting for hours, a quick walk around the house can sometimes settle that tight, crampy feeling. And if compression stockings have been recommended for you, wearing them on heavier or more swollen days can help too.
If the symptoms keep coming back despite all this, it’s a sign supportive measures alone aren’t enough- the next step is to work out the underlying cause and treat that properly.
The bottom line
Aching or crampy legs at night are common, but they’re not always harmless.
Muscle cramps and overuse are frequent culprits, but chronic venous insufficiency and varicose veins are among the most overlooked reasons for heavy, aching or crampy legs at night, especially when swelling or ankle skin changes are present.
Ready to get to the bottom of it?
If your night symptoms are becoming a pattern, especially if you’ve noticed swelling, visible veins, or ankle skin changes, it’s worth getting it properly assessed rather than guessing.
Dr Darryl Lim can evaluate your symptoms and, where appropriate, arrange a duplex ultrasound to check for venous reflux and identify whether your discomfort is coming from a treatable vein problem. Once you know the cause, you can stop trial-and-error and get a plan that actually fits your legs and your routine.
Frequently asked questions
Why do my legs ache or cramp more when I lie down?
When you’re still and distractions fade, symptoms can feel more noticeable- especially after a day of standing, muscle fatigue, or venous pooling.
Is night leg pain a sign of poor circulation?
It can be. Venous reflux can cause heaviness, swelling and crampy tightness. Arterial disease can cause rest pain (often in the feet/toes). The pattern helps differentiate.
When is leg pain at night dangerous?
Severe pain with a cold/pale foot, non-healing wounds, sudden one-sided swelling with redness/warmth, or breathlessness needs urgent assessment.
Can varicose veins cause cramps at night?
Yes. Venous insufficiency can contribute to heaviness, restlessness, and cramping in some patients, particularly after long standing days.