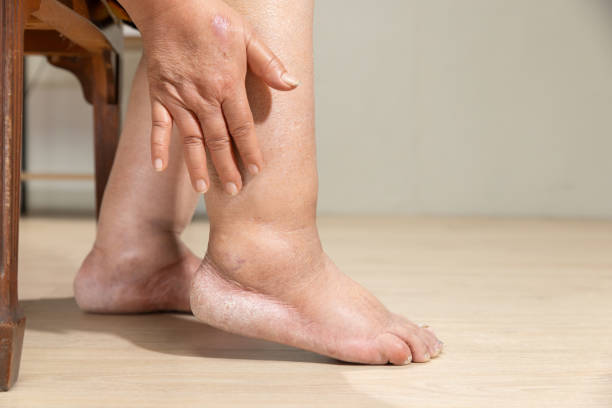
Swollen ankles can seem harmless at first. Maybe it happens after a long day on your feet. Maybe your shoes feel tighter at night. You elevate your legs and it settles…until the swelling returns the next day.
Ankle swelling (oedema) is common, but it’s not always “just fatigue”. Sometimes it reflects how your veins are coping. Sometimes can point to an issue with the heart, kidneys, liver, or a medication effect. The key is spotting the pattern and knowing when it deserves a proper review.
In this article, Dr Darryl Lim explains the common causes of ankle swelling, the red flags to watch for, and when a vein ultrasound can be useful.
What Causes Ankles to Swell?
Ankles swell when fluid collects in the soft tissues. Gravity pulls fluid to the lowest point, which is why swelling often shows up around the ankles first.
Swelling can involve:
- One ankle (unilateral swelling)
- Both ankles (bilateral swelling)
- The feet and lower calves
The cause matters. Some swelling settles overnight; other patterns suggest an underlying problem that deserves a proper review.
1)Chronic venous insufficiency (CVI)- one of the most common causes
Chronic venous insufficiency happens when the valves in the leg veins don’t close properly. Blood falls backwards (venous reflux) and pools around the ankles and calves, increasing pressure in the veins.
Why this causes swelling
When venous pressure rises, fluid can seep out of the small vessels into surrounding tissue. Over time this swelling becomes more noticeable, especially towards the end of the day.
Clues it may be vein-related
- Swelling that worsens by evening and is better in the morning
- Heaviness, aching, or “tired legs” after long standing days
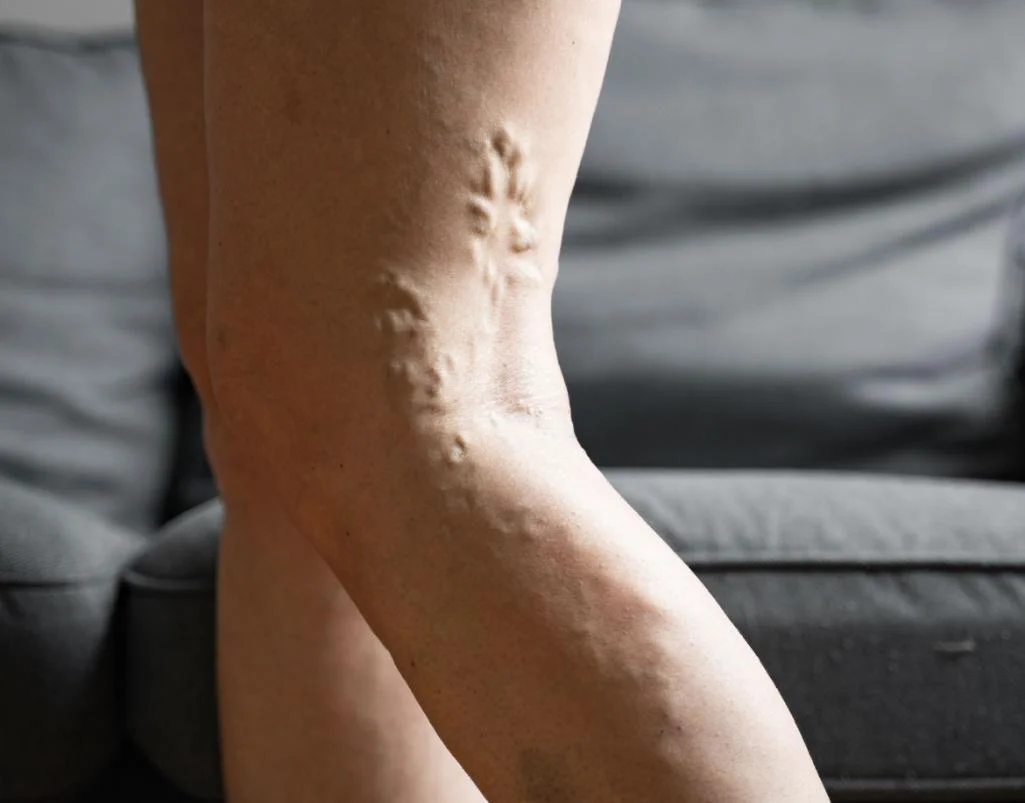
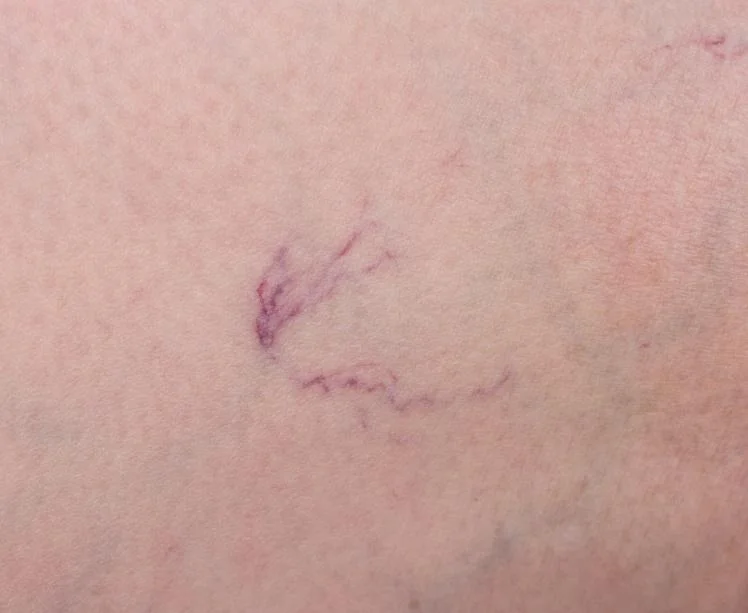
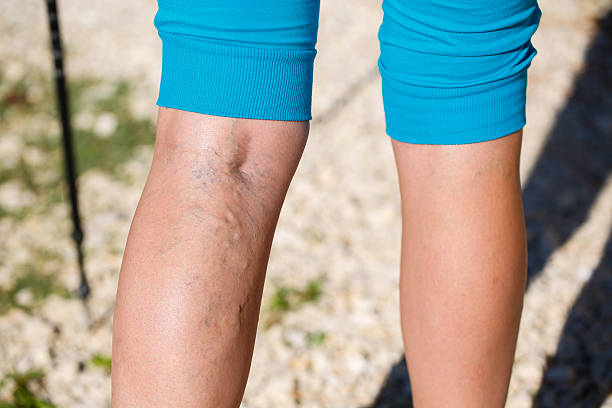
- Visible varicose veins or spider veins
- Itch, eczema-like patches (stasis dermatitis), or brown ankle staining
- Clear improvement when you elevate your legs
If your swelling follows this pattern, venous reflux is a common underlying cause.
2) Prolonged standing or sitting (gravity pooling)
Long hours standing (or sitting still at a desk) reduces the calf muscle pump and allows fluid to pool around the ankles.
This is common in:
- Nurses, teachers, retail staff
- Office workers who sit for long blocks
- Frequent travellers (long haul flights or drives)
In otherwise healthy people, this tends to settle overnight. If you’re swelling most days even after a good night’s rest, it’s worth looking for an underlying driver such as CVI, medication effects, or systemic causes.
3) Local injury, inflammation, or infection
A sprain, tendon irritation, arthritis flare, or cellulitis can cause ankle swelling. This is sometimes associated with pain, warmth, or redness. If the area is increasingly red, tender, or if you develop a fever, seek prompt medical review.
4) Pregnancy

Pregnancy increases blood volume, hormones relax vein walls, and the enlarging uterus can compress pelvic veins. The result is ankle swelling, particularly later in pregnancy.
Mild swelling can be normal. Seek prompt review if swelling is sudden, severe, one-sided, or associated with headache, visual changes, or high blood pressure concerns.
5) Weight gain
Extra body weight increases pressure inside the leg veins and can worsen venous pooling. It can also reduce daily movement, which weakens the calf pump.
Weight gain doesn’t “cause” vein valve failure on its own, but it can make swelling and heaviness show up earlier in the day and linger longer at night.
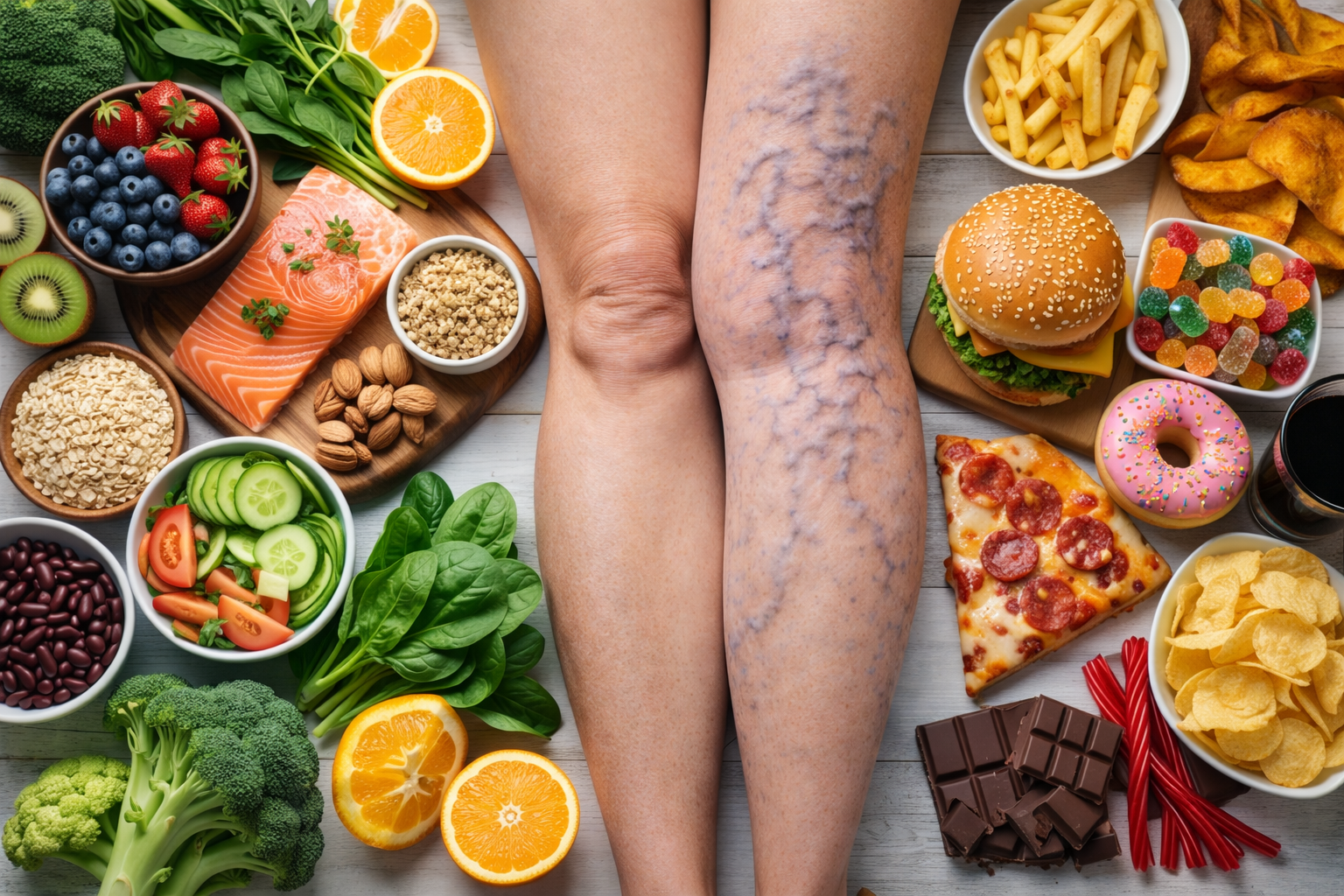
6) High salt intake (fluid retention)
Sodium makes the body retain water. Some people notice a very clear pattern: swelling is worse after restaurant meals, processed foods, or “salty days”.
If this is you, a simple experiment helps: reduce salt for 1–2 weeks and see if evening ankle swelling improves.
7) Heart, kidney, or liver conditions (systemic causes)
Systemic medical conditions can also cause ankle swelling, usually affecting both legs.
Heart failure- If the heart can’t pump efficiently, fluid backs up and pools in the legs.
Kidney disease- If kidneys aren’t clearing fluid and salt properly, swelling can build up.
Liver disease- Low protein levels (albumin) can reduce the body’s ability to keep fluid in the bloodstream, so fluid leaks into tissues.
Clues a systemic cause may be contributing:
- Swelling that is persistent and not clearly better in the morning
- Swelling higher up the legs (not just around the ankles)
- Shortness of breath, reduced exercise tolerance, fatigue, abdominal swelling, or reduced urine output
These situations need medical evaluation. The priority is often ruling out (or treating) systemic disease.
8) Lymphoedema (lymphatic swelling)
Lymphoedema happens when the lymphatic drainage system is not clearing fluid efficiently. It can be primary (rare) or secondary (for example after surgery, radiotherapy, infections, or longstanding inflammation).
Typical clues include:
- Swelling that may involve the foot and toes (sometimes with a “squared” appearance of the toes)
- A feeling of heaviness or tightness
- Skin that can become thicker over time
- Swelling that may be less responsive to simple elevation
Lymphoedema is managed differently from venous swelling, which is why an accurate diagnosis matters.
9) Deep vein thrombosis (DVT)- a medical emergency
A DVT is a clot in a deep vein. It classically causes sudden one-sided swelling, pain/tenderness, and sometimes warmth or redness.
Seek urgent assessment if you have:
- Sudden swelling in one leg (especially if it’s new or clearly asymmetric)
- Calf tenderness, redness, or warmth
- Unexplained breathlessness or chest discomfort (urgent)
DVT is less likely when swelling is longstanding and bilateral; but when the pattern is sudden and one-sided, don’t wait.
10) Medication side effects
Some medications can cause ankle swelling, including:
- Calcium channel blockers (a common blood pressure medication group)
- Steroids
- Certain diabetes medications
- Hormonal treatments
If the ankle swelling started after a medication change, please bring this up to your doctor. Sometimes the solution is as simple as adjusting the dose or switching to an alternative medication type!
How to tell if your ankle swelling is vein-related
Ankle swelling is more likely due to venous pooling (from CVI) if:
- It builds through the day and is worse at night
- You have leg heaviness/aching or visible varicose veins
- Elevating your legs noticeably improves swelling
- You have ankle itch, eczema-like patches, or brown discolouration
Venous swelling often creeps up gradually, and can be the first warning sign before more obvious skin damage appears.
When swollen ankles become concerning
Consider an evaluation if you have:
- Daily swelling that is persistent or worsening
- Itch, skin discolouration, or eczema-like changes near the ankles
- Wounds or ulcers around the ankle that heal slowly
- One leg consistently more swollen than the other
- Swelling plus pain, redness, or warmth
- Any swelling with shortness of breath
What happens if venous swelling is ignored?
If CVI is the root cause and pressure in the veins remain untreated, advanced cases of CVI may progress to developing:
- Brown pigmentation (haemosiderin staining)
- Venous eczema (stasis dermatitis)
- Skin thickening and hardening (lipodermatosclerosis)
- Venous ulcers
Once ulcers develop, treatment becomes more complex- which is why earlier detection and treatment when skin changes occur matters so much.
Need an expert vascular opinion for your Varicose Veins?
Book an appointment with Dr. Darryl Lim today and get a personalized treatment plan.
How swollen ankles are diagnosed
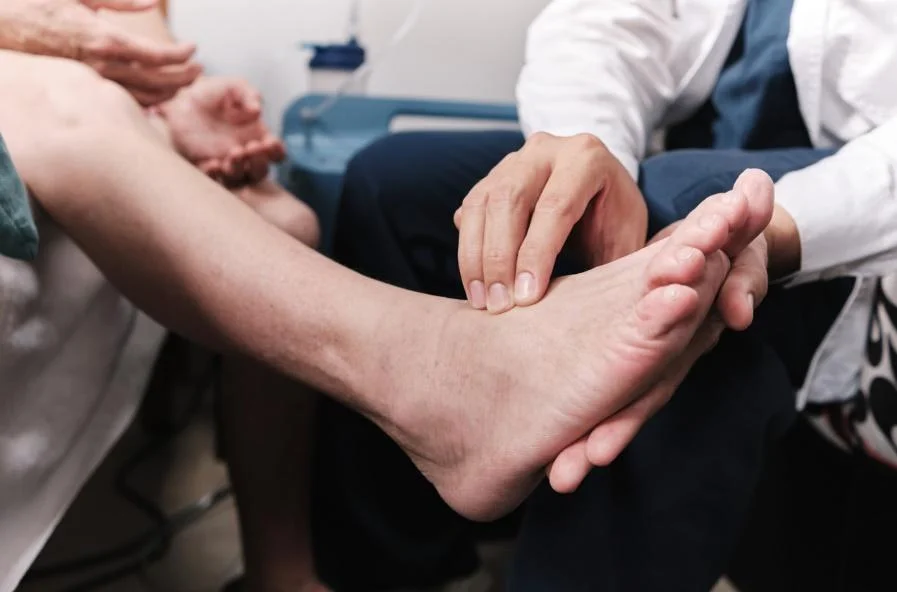
A proper assessment usually includes:
- Clinical examination (including pulses and a focused look at the skin)
- Review of medical history and medications
- Blood tests if systemic causes are suspected
- Duplex ultrasound if vein reflux or blockage is suspected
Duplex ultrasound is the gold-standard test to assess vein valve function and reflux. It helps confirm whether your swelling is primarily vein-related and guides treatment so you’re not guessing.
Simple steps that often help (while you arrange review)
If your swelling is mild and you’re otherwise well, these practical steps often reduce day-to-day discomfort:
- Elevate your legs for 15–30 minutes, especially in the evening
- Walk regularly (short, frequent walks are better than long periods of sitting)
- Break up long standing or desk time with calf raises and ankle pumps
- Moderate salt intake and stay well hydrated
- Consider properly fitted compression stockings if advised
If swelling persists despite these measures, supportive care alone is usually not enough. The aim is to identify and treat the underlying cause.
The Bottom Line
Swollen ankles are common, but persistent swelling isn’t something to ignore. Prolonged standing and salt intake can contribute, but in many adults the most common medical cause is chronic venous insufficiency especially when swelling is worse at night and accompanied by heaviness, varicose veins or skin changes.
If you’re seeing a pattern, it’s worth getting clarity early. Dr Darryl Lim can assess your symptoms and, when indicated, arrange for a duplex ultrasound to check for reflux or blockage.
Frequently asked questions
Is ankle swelling always a sign of poor circulation?
Not always. But circulation problems (especially venous insufficiency) are a common cause, particularly if swelling builds through the day and improves with elevation.
Why are both ankles swollen but not painful?
Bilateral swelling can be due to venous pooling, salt-related fluid retention, medication effects, or systemic causes (heart/kidney/liver). The pattern and associated symptoms help narrow it down.
When should I worry about ankle swelling?
Sudden one-sided swelling, redness, warmth, significant pain, or any swelling with breathlessness or chest discomfort should be assessed urgently.
Can compression stockings fix ankle swelling permanently?
Compression can reduce swelling and improve comfort, but it does not repair faulty vein valves. If reflux is present, treating the underlying cause is what provides longer-term relief.