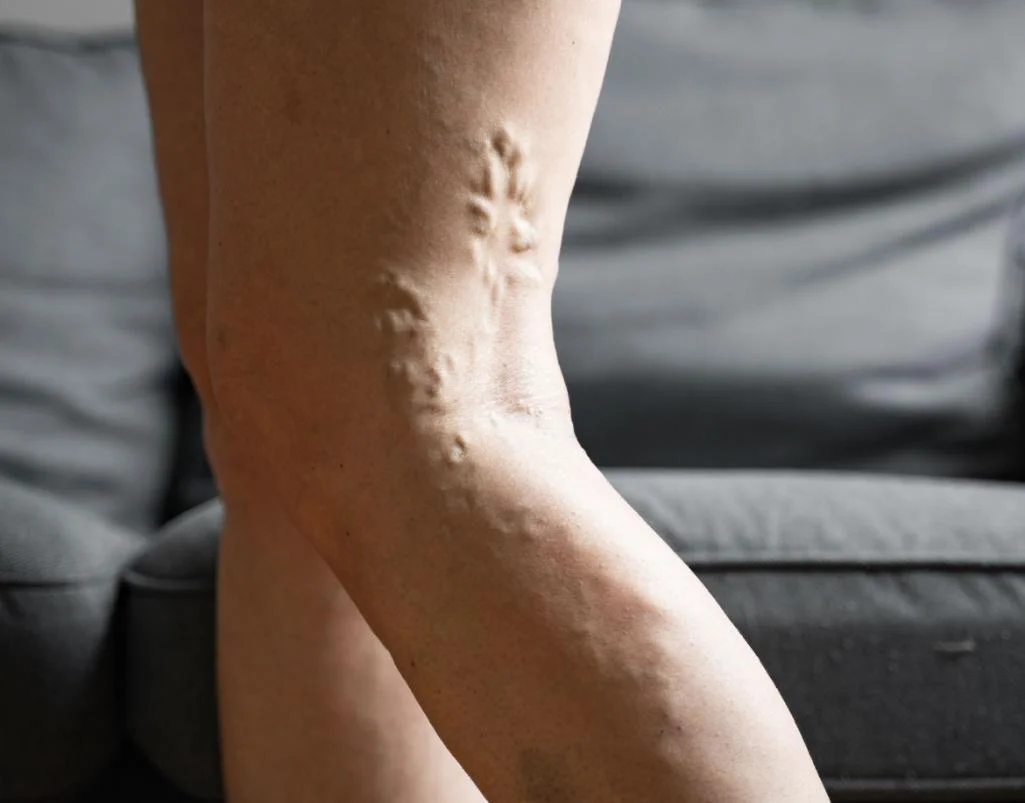
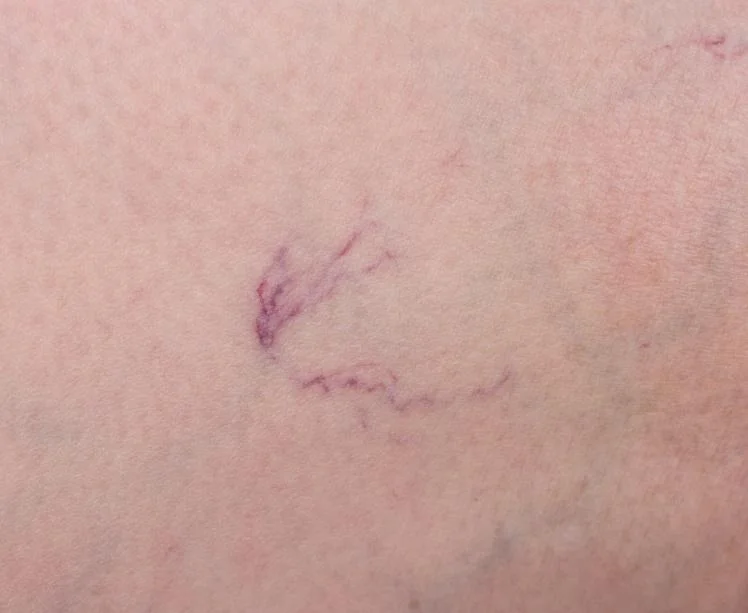
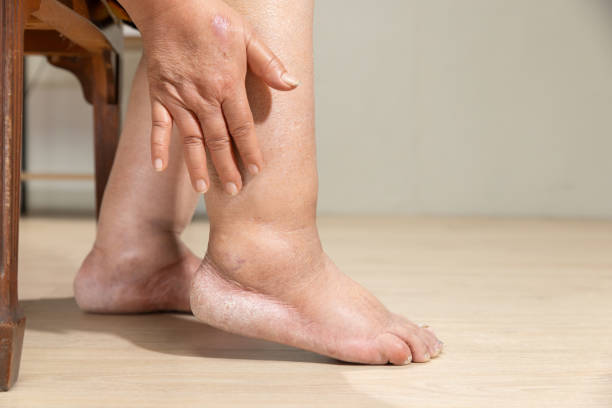
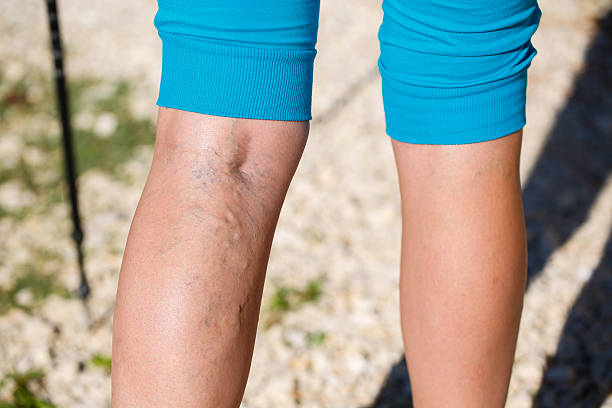
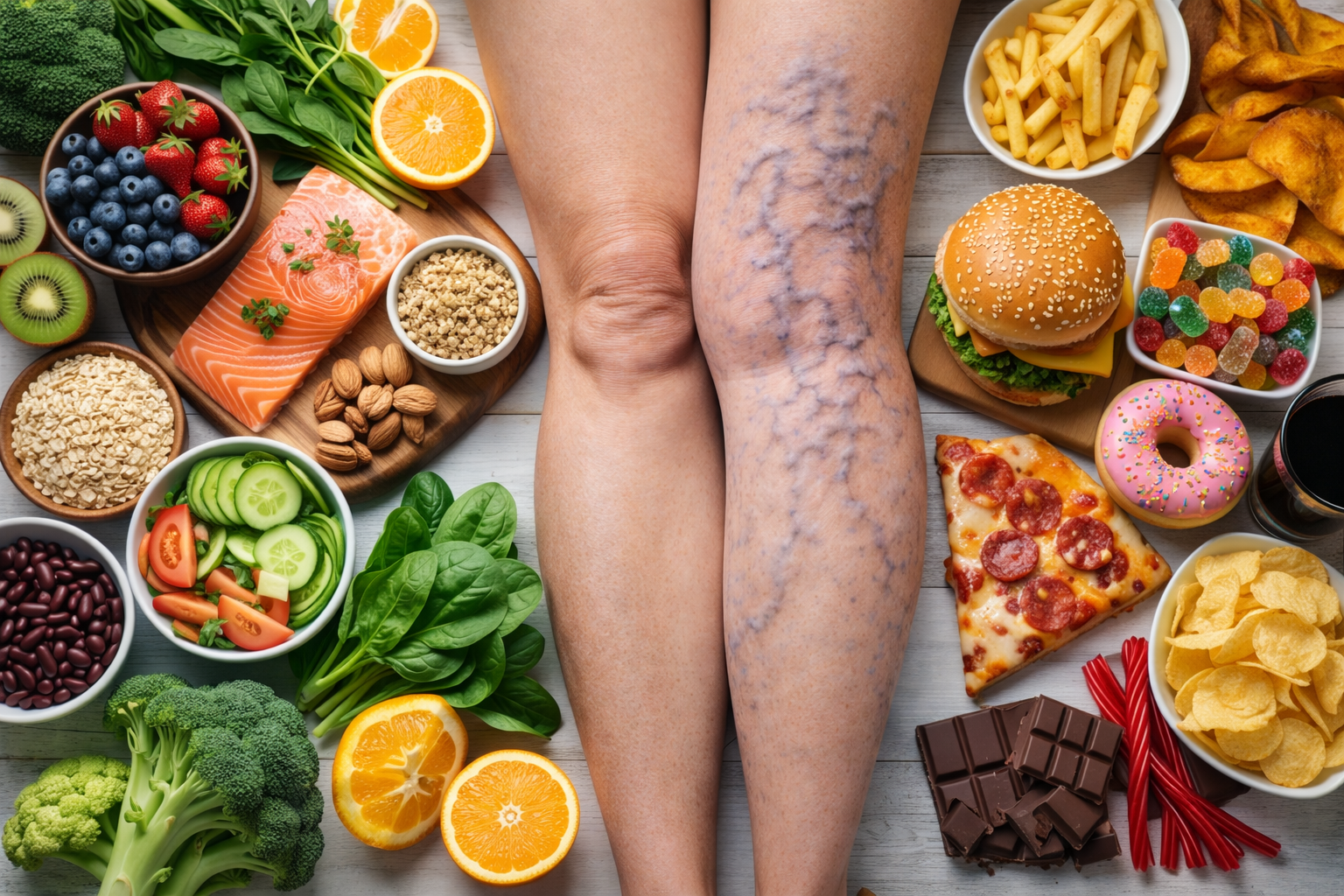
Varicose veins are common, especially in the legs. Most people think of them as a cosmetic issue, but when vein pressure builds up over time and the overlying skin becomes thin or fragile, complications can occur.
One question that understandably worries patients is: can a varicose vein burst?
Yes, it can. It is not the most common complication, but a varicose vein can rupture and bleed. When it happens, the bleeding can look dramatic because the vein is under pressure, especially if the leg is hanging down.
The important thing is knowing what to do immediately, and then getting the underlying vein problem assessed so it does not happen again.
In this article, Dr Darryl Lim, a vascular and varicose vein specialist in Singapore, explains why varicose veins can bleed, what warning signs to watch for, and what steps to take if it happens.
Can a varicose vein really burst?
Yes. A varicose vein can rupture, usually when high venous pressure combines with fragile skin overlying the vein.
This can happen in two ways:
- External bleeding: the vein bleeds through the skin. This is the more alarming situation because blood may flow steadily or splash if the pressure is high.
- Bleeding under the skin: the vein leaks into surrounding tissue, causing bruising, swelling, or tenderness.
External bleeding from a varicose vein can look frightening, but the first-aid steps are straightforward: pressure and elevation.
Need an expert vascular opinion for your Varicose Veins?
Book an appointment with Dr. Darryl Lim today and get a personalized treatment plan.
Why do varicose veins bleed?
Varicose veins develop when vein valves weaken. Instead of blood flowing smoothly upwards towards the heart, blood falls backwards and pools in the leg. This is called venous reflux, and over time it raises pressure inside the superficial veins.
A bleeding varicose vein usually happens because of a combination of factors.
1) High venous pressure
When blood pools in the lower leg, pressure builds up in the varicose vein. The more prominent and stretched the vein becomes, the more vulnerable it is to injury.
This is why bleeding often happens around the lower leg, ankle, or foot, where venous pressure is highest.
2) Thin or fragile skin
In more advanced venous disease, the skin over the vein may become thin, dry, inflamed, or easily damaged. Sometimes there is brown staining, eczema-like irritation, or a small scab overlying a prominent vein.
At this point, even a minor knock or scratch can trigger bleeding.
3) Scratching or minor trauma
Many patients with venous disease develop itching around the lower leg or ankle. Scratching may seem harmless, but if the skin is fragile and there is a pressurised vein underneath, it can be enough to open the skin and start bleeding.
Other common triggers include shaving cuts, bumping the leg, rubbing from footwear, or knocking the ankle against furniture.
4) Underlying Chronic Venous Insufficiency
Bleeding is more likely when varicose veins are part of underlying chronic venous insufficiency (CVI). Warning features include chronic swelling, brown ankle pigmentation, venous eczema, skin thinning, and previous ulcers.
In other words, bleeding is often not a random event. It can be a sign that the underlying vein disease has progressed.
Warning signs before a varicose vein bleeds
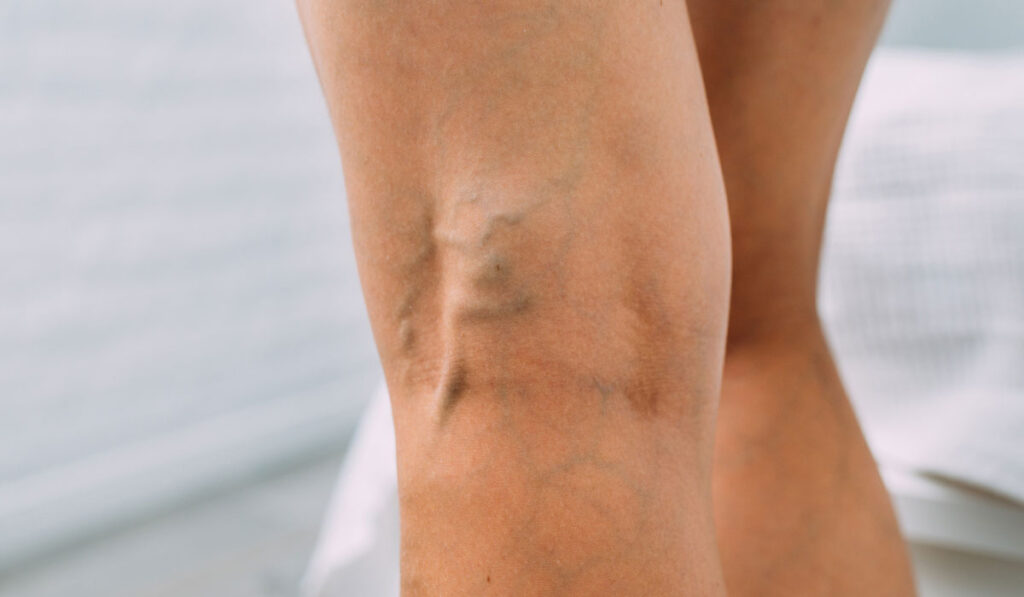
Not every bleeding episode gives warning, but many patients have clues beforehand.
Look out for:
- A large, bulging vein close to the skin
- Thin, shiny, or fragile skin over a vein
- A small scab or raw area overlying a varicose vein
- Persistent itching or irritation around the ankle
- Brown or purple skin discolouration
- Chronic ankle swelling
- Venous eczema or dry, inflamed skin
- A previous episode of bleeding from the same area
If you have these signs, it is better to get the vein assessed early rather than waiting for a bleeding episode.
What to do immediately if a varicose vein bursts
If a varicose vein starts bleeding, the main aim is to reduce pressure and stop the bleeding.
1) Lie down and elevate the leg
Lie down if you can, and raise the affected leg above heart level. This reduces venous pressure in the leg and helps slow the bleeding.
Avoid standing or sitting with the leg hanging down, because this increases pressure and can make bleeding worse.
2) Apply firm direct pressure
Use a clean cloth, towel, gauze, or dressing and press firmly over the bleeding point.
Keep the pressure continuous. Do not keep lifting the cloth to check whether it has stopped — that can restart the bleeding.
3) Keep pressure on for several minutes
Hold steady pressure until the bleeding stops. If the cloth becomes soaked, add another layer on top rather than removing the first layer.
4) Seek medical attention even if it stops
Once bleeding is controlled, the episode still needs proper medical review. The immediate bleeding may have stopped, but the underlying reflux and high venous pressure may still be present.
That is why bleeding can recur if the vein problem is not addressed.
What not to do
A few common reactions can make bleeding worse.
Do not:
- Stand up or walk around with the leg down
- Keep removing the dressing to “check”
- Apply only a loose tissue or plaster without firm pressure
- Ignore the episode once bleeding stops
- Delay help if bleeding is heavy or you feel faint
If bleeding is heavy, does not stop with firm pressure, or you feel dizzy, faint, short of breath, or unwell, seek emergency care immediately.
Is a bleeding varicose vein dangerous?
It can be. Many episodes are controlled with proper first aid, but a bleeding varicose vein should still be taken seriously. The bleeding may look minor at first and then recur. In older patients, patients on blood thinners, or those living alone, bleeding can be more dangerous.
Possible risks include:
- Significant blood loss
- Recurrent bleeding from the same vein
- Infection if the skin is broken
- Progression to venous ulcers
- Ongoing venous hypertension if reflux is untreated
The key point is this: stopping the bleeding is only the first step. Preventing the next bleed requires treating the underlying cause (usually venous reflux).
Why bleeding can happen again
A plaster may cover the skin, but it does not reduce the pressure inside the vein.
If the vein remains enlarged and refluxing, the same weak point can reopen. This is especially true if the skin is thin, itchy, inflamed, or already damaged.
This is why patients with bleeding varicose veins should have a proper vein assessment, even if the bleeding episode seemed to settle quickly.
How to reduce the risk of a varicose vein bursting
If you have large surface veins, fragile skin, or previous bleeding, prevention matters.
Treat varicose veins before complications develop- Early treatment reduces venous pressure and lowers the risk of skin damage, ulceration, and bleeding. If you already have skin changes or bleeding, assessment becomes more urgent.
Protect the skin- Avoid scratching, aggressive rubbing, or shaving directly over prominent veins. Use gentle moisturisers if the skin is dry or irritated.
If there is venous eczema, brown staining, or a small scab over a vein, do not ignore it.
Manage swelling- Leg elevation, walking, and compression stockings may help reduce swelling and pressure. Compression should be properly fitted and used appropriately, especially if there are wounds or other circulation concerns.
Avoid prolonged immobility- Long periods of standing or sitting allow pressure to build in the lower legs. Short walks, ankle pumps, and calf raises help activate the calf pump and improve venous return.
How bleeding-risk varicose veins are assessed
A good assessment looks beyond the visible bleeding point. The goal is to identify the reflux source causing high pressure in the first place.
Dr Lim will usually assess:
- The location and pattern of visible varicose veins
- Any skin thinning, eczema, pigmentation, or ulcer risk
- Previous bleeding episodes
- Swelling and symptoms of chronic venous insufficiency
- Whether there are signs of deeper venous disease
The key investigation is usually a duplex varicose vein ultrasound scan, which checks valve function and maps areas of venous reflux. This allows treatment to target the true source of pressure rather than simply treating the surface vein that happened to bleed.
Treatment options to prevent recurrence
Treatment depends on the ultrasound findings, the vein pattern, and the condition of the skin. The aim of treatment is not just cosmetic improvemenm but to reduce venous pressure, protect the skin, and prevent repeat bleeding.
Options may include:
Endovenous thermal ablation (Radiofrequency Ablation)
Radiofrequency ablation or laser ablation can be used to close a faulty refluxing vein, reducing pressure in the varicose branches.
Medical Adhesive “Glue” Closure (VenaSeal)
In selected cases, medical adhesive can close the diseased vein without heat-based treatment.
Ultrasound-Guided Sclerotherapy
This may be useful for certain refluxing branches or smaller veins, particularly when there are localised bleeding-risk areas.
Prominent surface varicose veins may sometimes be removed through tiny punctures, depending on anatomy and the overall treatment plan.
When should you see a vascular specialist?
You should seek evaluation if you have:
- Any episode of bleeding from a varicose vein
- A scab or fragile skin over a visible vein
- Large, bulging varicose veins near the ankle or foot
- Persistent ankle swelling
- Brown skin discolouration or venous eczema
- Previous venous ulcers
- Recurrent itching or irritation over varicose veins
If you have already had a bleeding episode, it is better not to wait for it to happen again. Dr Darryl Lim can assess the vein pattern and arrange ultrasound mapping where appropriate, so a treatment plan can be built around the underlying reflux.
The bottom line
Yes, a varicose vein can burst. It usually happens when high venous pressure meets thin, fragile skin.
If it happens, lie down, elevate the leg, and apply firm direct pressure. If bleeding is heavy, persistent, or you feel faint or unwell, seek emergency care.
Even if the bleeding stops, the underlying vein problem still needs attention. A proper assessment and duplex ultrasound can identify the reflux source and help prevent future bleeding, skin damage, and ulcers.
Need an expert vascular opinion for your Varicose Veins?
Book an appointment with Dr. Darryl Lim today and get a personalized treatment plan.

Frequently asked questions
Can a varicose vein burst suddenly?
Yes. It can happen suddenly, especially if the vein is large, under pressure, and covered by fragile skin. Sometimes it follows a minor scratch or knock.
Is a burst varicose vein an emergency?
It can be, if the bleeding is profuse. If bleeding is heavy, does not stop with firm pressure, or you feel faint or unwell, seek emergency care. Even if bleeding stops, vascular review is still recommended to fix the underlying cause.
How do you stop bleeding from a varicose vein?
Lie down, raise the leg, and apply firm direct pressure over the bleeding point with a clean cloth or dressing. Keep pressure on continuously for several minutes.
Can a bleeding varicose vein happen again?
Yes. If the underlying reflux and high venous pressure are not treated, bleeding can recur.
How can I prevent varicose veins from bursting?
Protect fragile skin, manage swelling, avoid scratching, use compression if advised, and seek treatment for significant varicose veins or skin changes.
Should I see a specialist after one bleeding episode?
Yes. One bleeding episode is enough reason for vascular assessment, because it may indicate advanced venous disease and a risk of recurrence.